HIV numbers stay high in Saskatchewan
- Angela Hill | December 09, 2017
Danita Wahpoosewyan, from Sakimay Frist Nation, was in Ottawa as part of an Indigenous response to HIV and AIDS and the kick off to Aboriginal AIDS Awareness Week.
“I see the need for more voices from Saskatchewan because of high rates [of HIV] in Saskatchewan,” said the Canadian Aboriginal AIDS Network (CAAN) board member by phone on Dec. 1.
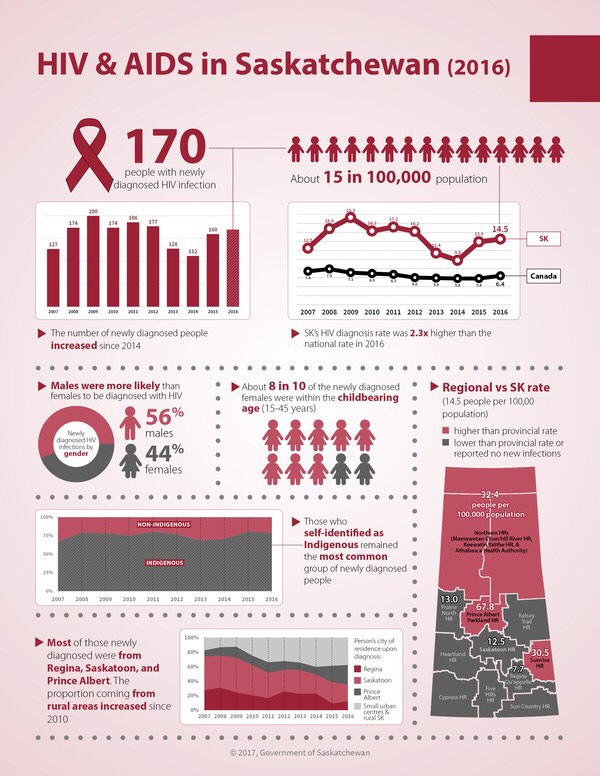
Saskatchewan continues to have a rate of new infections that is more than twice the national average. Newly released provincial numbers from 2016 show 170 people in that year were diagnosed with HIV.
According to CAAN, Indigenous communities continue to be over-represented in the HIV statistics – 2.7 times higher than other Canadians.
“I see too many of my people, they are dying,” said Wahpoosewyan, who is an HIV peer mentor with Regina Qu’Appelle Health Region and co-facilitates the Anyone at Risk Support Group at AIDS Programs South Saskatchewan.
“Stigma and discrimination plays a huge role because people don’t want to get tested.”
She has heard stories of people leaving reserves because they feel they are not accepted.
“Being positive is not a good thing in my community,” Wahpoosewyan said.
She said she has heard people say, “’if I get tested and I am positive I am going to kill myself.’” When people do finally decide to get tested it is too late and they are very sick, she said.
Related: Doctors call for HIV state of emergency in SK
Numbers released by Saskatchewan’s Ministry of Health show the vast number of new cases are from the Prince Albert Parkland and Sunrise Health Regions, and the northern health regions and authorities.
“We want a more robust public discussion among First Nations leaders about the stigma of HIV in their communities as this remains one the main reasons we continue to see late diagnoses, advanced disease and AIDS death,” said Dr. Kris Stewart by email. He is an internal medicine physician with focus on HIV, HCV and TB, and a co-lead of the Saskatchewan HIV/AIDS Research Endeavor (SHARE).
In late 2016, Wahpoosewyan joined to a group of doctors, including Stewart, calling on government to declare a public health state of emergency and increase funds to tackle HIV.
There were mixed results, Stewart said. The Saskatchewan government adopted the global 90-90-90 strategy, which sets three measures of progress – 90 per cent of people tested, 90 percent of the people who test positive on treatment, and 90 of those being treated with supressed viral load.
“There is improved engagement with clinicians from the ministry, but no new money,” Stewart said.
They want to see something like the Saskatchewan surgical initiative.
“This is great example of how we can be effective and we can be leaders if we make something a priority. Why elective knee and hip replacements and not HIV prevention?” he wrote.
The doctors want to see funding for universal coverage of medication so no one goes untreated, more outreach workers, and staff dedicated to deal with the high number of HIV positive women who are pregnant or at risk of becoming pregnant and HIV positive.
When Wahpoosewyan tested positive for HIV, she “took it as an opportunity for myself to grow,” taking care of her health and learning her culture.
“It’s not a death sentence, it’s not a bad thing. It’s manageable,” she said.
She has advice.
“Get tested. If you find out you are positive, take the steps to get healthy.”
The mother of two and grandmother of nine looks at her 70-year-old parents and 90-year-old grandparents as where she wants to be.
“I’m 51 years old right now and I know as long as I take my medications I am going to be an old lady, I am going to live a long life.”